By Roxanne Squires
NEW YORK – Patient- and family-centered care is embedded into the design of the new 740,000-square-foot NewYork-Presbyterian David H. Koch Center, an ambulatory care center that combines innovative clinical approaches and cutting-edge technology to provide exceptional care and a seamless patient experience.
The architectural design of the new David H. Koch Center is the result of collaboration among HOK as architect, Ballinger as medical architect, and Pei Cobb Freed & Partners as consulting architect for building envelope and lobby; with the team beginning excavation in August 2014 and wrapping up the project April 2018.
NewYork-Presbyterian and physicians from Weill Cornell Medicine were also actively involved throughout the planning process.
The $1 billion center provides interdisciplinary treatment for outpatient surgery, endoscopy, interventional radiology, diagnostic imaging, radiation oncology, infusion, and digestive disease treatments.
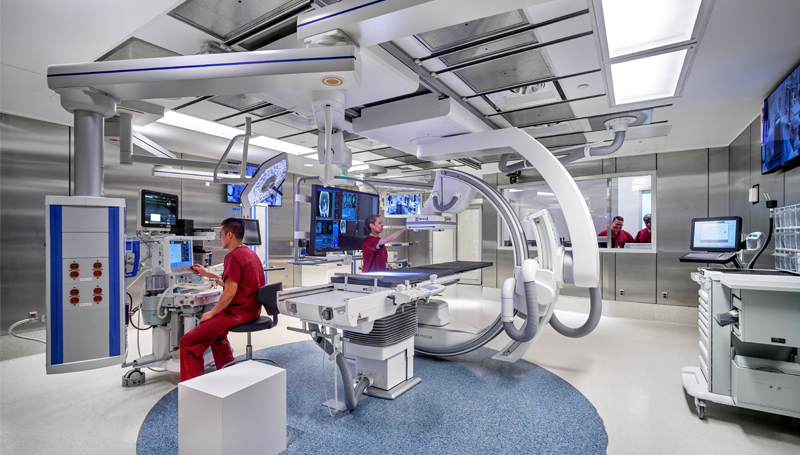
Additional clinic features include 12 operating suites, six interventional radiology procedure rooms and 11 endoscopic procedure rooms.
As the center focuses on the human experience, the program provides a comprehensive set of services for patients in a contemporary and soothing environment.
The high performance building facade includes 225,000-square-feet of a triple-glazed insulated curtain wall with an integrated internal obeche wood screen and a silk-screened frit on inside of the outer layer creates an undulating pattern. The curtain wall not only contributes to the performance of the building – but also creates a warm and inviting face to the community, and a distinctive and rich architectural character.
According to Erin Nunes Cooper, associate principal, Ballinger, critical building systems and infrastructure that are essential to maintaining building operations during an emergency are located above grade to protect and isolate them from the impacts of storms, floods and other hazards.
A green roof covers 30 percent of the roof’s surface, which helps cool the building and reduce the heat island effect. It is also capable of retaining up to 6 inches of storm water for slower release back into the sewers and helping to alleviate pressures on the city’s storm sewer system.
The infusion and radiation oncology program, located on the 4th floor of the building, offers three radiation therapy rooms including two linear accelerator rooms and New York’s first MRI-guided linear accelerator room are used for precision radiation treatment of tumors. These spaces are protected with lead and concrete, and are typically located in basement areas. By locating the treatment rooms on the 4th floor of the building, patients and staff are elevated and have access to natural light.
All of the prep/recovery positions are private rooms, serving as designated spaces for the patient and their family for the duration of their stay.
The rooms are fully enclosed with sliding glass doors, instead of the more traditional three walls and a curtain. Patients change, prep, recover and check out in their assigned room. The room provides a secure storage space for the patient’s belongings as well as a private waiting space for the patient’s family members during the procedure. Patients even prep and recover with the same nurse and care team.
Furthermore, three prep/recovery rooms are dedicated to each procedure room, which allows for greater consistency and continuity of the care team for each patient. Dedicated rooms also make it easier for caregivers and clinicians to find family members for face-to-face updates and instructions on follow-up care. These patient rooms were designed to maximize access to natural light, which has been shown to benefit patient outcomes.
Decentralized stations are located outside pairs of prep/recovery rooms, one of the first applications in the country in an ambulatory procedure environment. The care teams committed to eliminating the central nurse station entirely. Instead, a single Central Command Center is located at the juncture of the procedure platform, which monitors all activities between the procedure platform and prep/recovery zone. The result is that all caregivers are able to spend more time either in the patient rooms or at the decentralized stations in close proximity to the patients.
Circulation is clear, with a separation of “on-stage” and “off-stage” flows so patients and families can travel along the light-filled perimeter corridors with clear wayfinding, and staff can move efficiently through the building, minimizing disruption to guests.
A fully integrated art program throughout the building hosts a diversity of works at key locations as positive distractions for patients undergoing medical treatment. A warm material palette that carries the wood features indoors creates a soothing environment that facilitates anxiety reduction.
The team also conceived of a procedure experience without waiting and choreographed a patient experience that uses technology to streamline the process. Patients are pre-registered and are greeted by patient ambassadors upon arrival. Kiosk check-in is available in the lobby, and all patients and their families or companions receive a wrist band at check in and are directed to the appropriate floor.
Care team members are notified when the patient arrives in the building, allowing them to greet the patient on the floor and escort them directly to their dedicated procedure room. Electronic notifications are used to communicate with family members during or after the procedure so that they can comfortable comfortably leave the floor knowing that they can return during the patient’s recovery.