Humidification systems designed for large buildings help maintain consistent indoor humidity in healthcare environments with high air volumes and continuous operation. | Photo Credit (all): Courtesy of DriSteem
By Dave Schwaller
Infection prevention is a top priority in healthcare. Ventilation rates are defined down to the air change. Filtration levels are closely tracked. Pressure relationships are monitored and tested. These controls are well established in healthcare design and day‑to‑day operations.
Humidity control, however, is often treated differently. It is usually present but not always managed with the same level of intent or attention as other environmental controls.
Research referenced by ASHRAE and the CDC indicates that maintaining indoor relative humidity between 40 and 60 percent helps reduce airborne transmission risk and supports occupant health. When humidity control is not actively addressed, even well‑designed infection prevention strategies can lose an important layer of support.
Where Humidity Control Breaks Down and Why It Matters
High air change rates, continuous HVAC operation, and aging infrastructure all make precise humidity control more difficult in real‑world operation. As a result, indoor relative humidity in many healthcare facilities falls below recommended levels. When humidity control is not consistently maintained, several risk factors tend to appear together.
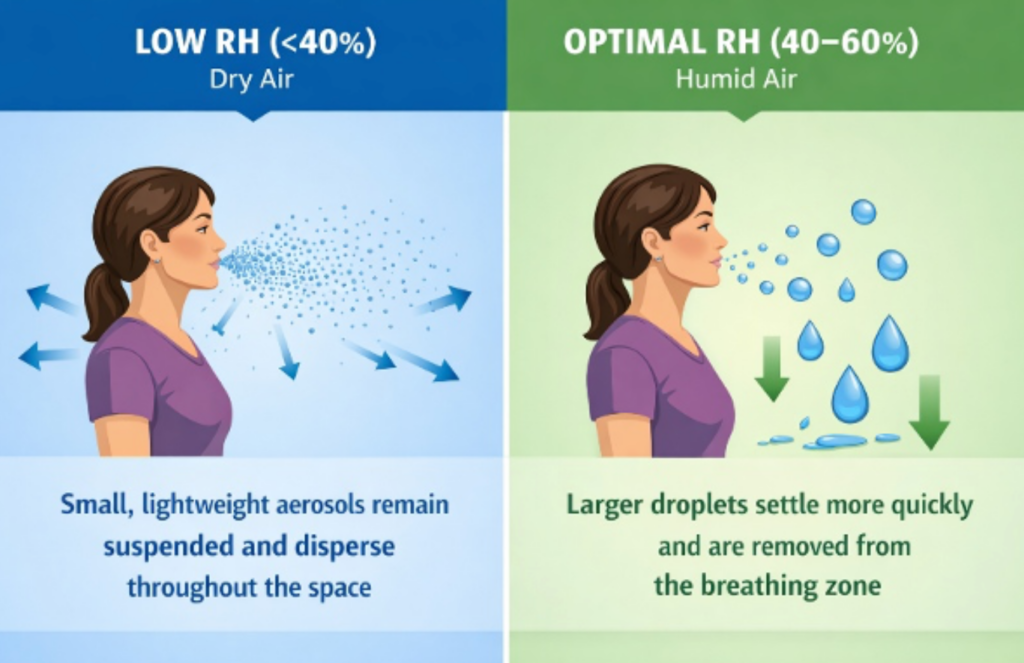
Dry air causes respiratory droplets to evaporate quickly, forming smaller particles that can remain airborne longer and travel farther. Some pathogens also persist longer in dry environments. At the same time, low humidity dries out mucous membranes in the nose and throat, reducing the body’s ability to trap and expel contaminants.
These effects are easy to miss because they rarely trigger alarms or immediate failures. Over time, however, they can increase infection risk, affect patient outcomes negatively, and contribute to higher staff illness rates.
Humidity control also plays a direct role in equipment reliability, building durability, and the performance of medical materials and supplies.
Dry air increases the likelihood of electrostatic discharge in sterile processing areas, imaging suites, and other spaces with sensitive electronics. It also accelerates wear on the building itself. Flooring, millwork, and finishes tend to degrade faster under dry conditions, driving up maintenance needs. Medical equipment is affected as well, as prolonged dryness can contribute to performance issues and reduced service life.
Medical materials and supplies are impacted too. Extended exposure to low humidity can compromise sterile packaging, shorten the usable life of certain disposables, and create static‑related handling challenges. Over time, these conditions increase waste and add hidden costs to materials management.
The Hidden Costs of Poor Humidity Control
Maintenance costs rise as equipment and finishes wear out faster than expected. Energy use is another concern, as comfort complaints often lead to increased heating or ventilation, which can further reduce humidity while adding energy load.
The greatest disruption often comes from reactive solutions. Portable humidifiers and temporary fixes may address symptoms, but they are rarely efficient or reliable long term. Facilities with well‑designed, centrally managed humidity control systems typically see fewer interruptions and more predictable operating costs.
Evaluating humidity control strategies in healthcare

When healthcare facility leaders evaluate humidity control options, first cost should be only one consideration.
Both steam and adiabatic humidification systems are used successfully in healthcare when properly selected, designed, and maintained. Steam humidification is commonly chosen when precise control is essential, while adiabatic systems are often used when energy efficiency is a priority and strong water management and maintenance practices are in place.
Regardless of technology, evaluation should focus on long‑term performance. Key questions include:
- Can the system maintain target relative humidity under real operating conditions?
- How will water quality be managed over time?
- What staffing time and maintenance are required?
- How will performance be monitored and documented?
In healthcare environments, long‑term reliability and maintainability often matter more than initial cost.
Project Examples: Lessons from hospital and Senior Care Facilities

Two DriSteem projects illustrate how intentionally designed humidity control can support patient health, staff performance, and system reliability across different healthcare settings.
At a large hospital in Buffalo, New York, aging air handlers serving operating suites, sterile processing, the pharmacy, and patient areas were replaced in phases to avoid interrupting critical operations. A key lesson from the project was the value of clean humidification steam. The hospital selected a steam-to-steam humidification system that used boiler steam as the energy source to generate humidification steam from fresh water. By treating humidity control and air purity as integral to the HVAC upgrade, the facility strengthened its environmental control strategy at a time when operational reliability mattered most.
A similar lesson emerged at a skilled nursing facility in Michigan’s Upper Peninsula, where a major renovation introduced 100 percent outdoor air and higher indoor temperature setpoints to support resident comfort and health. These conditions significantly increased humidification demand. Steam humidification was installed to help reduce the risk of virus transmission for a vulnerable population. The project reinforced an important takeaway for senior care environments: humidity control is not a comfort feature, but a critical component of resident safety, infection prevention, and long‑term operational performance.
Making Humidity Control Part of Infection Prevention
Effective humidity control belongs alongside ventilation, filtration, and pressurization as a core element of environmental control. On its own, it will not eliminate the risk of infection. But when humidity is managed intentionally rather than left to chance, it strengthens the overall system. In healthcare environments where patient safety, staff performance, and operational resilience are tightly connected, humidity control is more than a comfort consideration. It is a fundamental part of doing the job well.
Dave Schwaller is an Application Engineer with DriSteem.


