Strategies to Help Hospitals Run Efficiently During COVID-19
By Samuel Jackson PE, LEED AP
According to the government policy watchdog website, TheHill.com, more and more governors across the United States are instructing state health officials to increase bed capacity to meet the expected surge in COVID-19 patients. As a result, many healthcare leaders are effectively working two jobs right now. Not only are leaders fulfilling their usual day-to-day responsibilities, but leaders are also focusing on how they’re going to modify their existing operations and facilities to care for COVID-19 patients.
Hospitals are looking for effective, efficient strategies and solutions that can be implemented quickly to keep patients safe and protect the caregivers and medical professionals on the front lines battling this disease. It’s important that our medical professionals are safe throughout this pandemic. With appropriate PPE clothing, doctors should be kept fairly safe. Additionally, distance tape should be used to help to keep people at least 2 meters apart at all times. Marking it out with this tape will help to remind people and make it clear where they should and shouldn’t be. As well as this, all people working in hospitals all over the world should have access to hand sanitizer at all times so they can kill any bacteria on their hands. Luckily, hospitals in the UK have strong supplies of hand sanitizer thanks to companies like phs Direct. For those who don’t know, phs Direct are the UK’s leading supplier of commercial wholesale hand sanitiser, helping to keep offices, workspaces and businesses as a whole up to vigorous hygiene standards. This is helping many people stay safe from COVID19. In contrast, hospitals in the US are only just starting to catch up with those in the UK. US officials are finally beginning to realize the problem that coronavirus is causing worldwide.
Here are several key issues to consider and strategies for leaders to address the unique aspects of the novel coronavirus.
Understand air handling issues regarding isolation spaces. As with any airborne infectious disease, COVID-19 patients need to be isolated to protect the health of other individuals in the facility. Since most hospitals only have a few isolation rooms, the influx of COVID-19 can be problematic. The air handling requirements to create additional isolation spaces fall into three categories, each with their own issues that are important to be aware of:
- First, 100% exhaust air is required. As with any airborne infectious isolation room (AIIR), the air in a COVID-19 patient room should not be recirculated. To conserve energy, most hospitals are designed to intake 25% of outdoor air and recirculate the remaining 75%. To achieve 100% intake of outdoor air poses a significant issue, as most hospital facilities do not have an infrastructure designed with this capability. It is important to conduct a thorough analysis of the hospital’s existing heating, cooling, fan output and controls. The total system impacts need to be understood and considered before attempting to increase isolation spaces. This is a difficult issue but one that is absolutely necessary in the case of COVID-19.
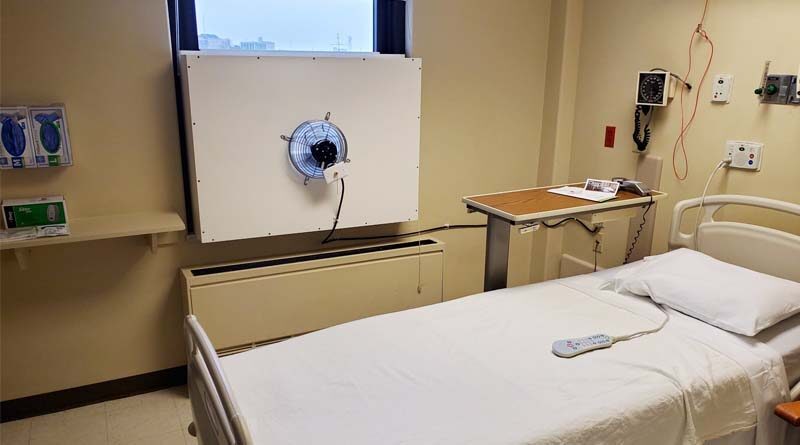
- Second, it is important to create a negative pressure in an isolation room to protect the other patients and staff in the hospital. Since the supply air to the room is typically designed to the code minimum, creating a negative pressure must be controlled through the exhaust system. Creating a negative space in the patient room on a temporary basis can be simple if the facility is willing to take out the window and put in what is basically a fan, blowing air out of the building. This will meet the code requirements for a temporary response. Creating a negative space is tricky because of the pressure relationship to certain rooms. If you make a change to one room, leaders could disturb other air change relationships.
- Finally, try to increase the amount of outdoor air to as close as 100% as possible. However, this poses issues. It is critical that leaders consider the ambient air temperature of outdoor air. If the air handlers are not sized appropriately to manage large intakes of cold air, they could freeze. Similarly, if the air is humid, and the air handlers do not have enough capacity, this may impact the ambient temperature within the isolation rooms as well.
Monitor. Monitor. Monitor. COVID-19 patients are in acute respiratory distress and require significant amounts of oxygen and medical gas supply for ventilators. As facilities start doubling up patients on ventilators, medical gas usage can increase significantly. It is important that leaders assign an individual to monitor the following on an ongoing basis:
- Bulk oxygen levels. When does the system need to be filled? Has this been scheduled?
- Med gas supply. Are there any supply chain issues? Are the current providers operating as usual, or has their delivery schedule been affected?
- Fuel oil levels. Are there enough fuel reserves to last a few days in case of inclement weather or if the facility has a power outage?
- Air filters. With the potential change in air flows, it’s essential to make sure all of the air filters have been replaced to limit the load on the air handler.
- Is there a sufficient supply of salt for the water softeners?
- Water treatment. Is the water treatment vendor able to maintain service?
Implement a formal checklist. The patient surge due to COVID-19 has changed how hospitals operate on a daily basis. Items that were once addressed on a weekly or monthly basis, now need to be checked daily. Keeping track of what leaders are responsible for can easily fall through the cracks, especially in light of quarantines and staff changes. Since there are still only 24 hours in a day, leadership does not always have time to focus on everything. A thorough checklist can be beneficial in times like this. Not only does it serve as a reminder for those in charge, but it also makes it easy to delegate individual tasks to others.
Limit the spread of coronavirus in surgical areas. As facilities are scrambling to create isolation units for COVID-19 patients, leaders are also preparing for other likely scenarios, such as how they perform surgery on an infectious patient. By code, operating rooms are required to be positive airflow. There are no exceptions to this rule. How does a hospital limit the spread of coronavirus if they have to put a patient in a room that is required to be positive, which is contrary to the current infection control measures? The following is a list of considerations:
- Do the procedure when no other surgeries are occurring in other operating rooms that are served by the same air handling unit (AHU).
- Use an operating room at the end of the OR suite corridor to contain the virus as much as possible.
- Put the AHU into 100% outdoor air mode if possible. If the unit does not stay on due to low limit temperature safeties, allow only as much return air as required to keep the AHU running. Operating room air handlers must have HEPA air filters. The CDC recommends not recirculating air unless it is HEPA filtered.
- If possible, put one of the temporary construction enclosures around the operating room door to the corridor and put a portable HEPA filter unit inside this enclosure.
- After the surgery is over, flush the air in the area served by the OR AHU for 60 minutes.
Recognize limits of HEPA filters. The CDC allows recirculated air as long as it goes through a HEPA filter, but it is important to remember that not all air handling units are large enough to push through a HEPA filter. There is some research that indicates that the coronavirus is small enough to pass through a HEPA filter. To err on the side of caution, consider blocking off access to areas where HEPA filters exhaust such as parking garages or spaces between buildings.
Communicate internally and externally. These are extraordinary times and call for extraordinary measures. The patient load at hospitals is changing daily, reaching unimaginable surge levels. While it is busy and lives are at stake, it is important that hospital leaders commit to a quick daily “huddle” with key departments to review status of key areas. Similarly, it is important to keep an open dialogue with all of the authorities having jurisdiction including the local Department of Health and the Joint Commission. To meet the surge requirements, many temporary renovations are being done, including some that may not be allowed by code. By keeping in continuous conversation with officials, explaining what measures have been taken, can help keep everyone on the same page. If hospitals have social media pages, then keeping the local community informed via those would also be a good idea. There are some recommendations on Violet PR that could be useful to many businesses, as well as hospitals.
In the modern era, the world has never experienced a time such as this. The global healthcare industry has been thrust to the frontlines of a viral pandemic battling an evasive and fast-moving enemy (COVID-19). The first quarter of 2020 may well be the greatest peacetime effort in innovative thinking the US, and the world has ever seen. The global coronavirus pandemic has affected everyone from teachers learning how to use e-learning full-time to everyone in the service industry learning how to work in isolation.
The industry is more equipped today than at any time in human history to handle such a battle with its enhanced technology, Lean operations, sophisticated air handling systems, and evidence-based medicine that facilitate life-saving care. The collective goal is to respond quickly – with Effective and Efficient COVID-19 Strategies… Right Now – so that we might stay ahead of this virus, reduce the spread, and allow modern medicine to save lives. Unfortunately, lots of people have contracted COVID-19 already, particularly in busy cities. For example, there are thousands of cases in NYC, which is why lots of people are choosing to contact places like this NYC COVID-19 Attorney. Seeking legal compensation is completely optional though. Just make sure you get the compensation you deserve.
Samuel Jackson, PE, LEED AP, is Director of Engineering with BSA LifeStructures. He can be reached at sjackson@bsalifestructures.com.